Depression and Income
Socioeconomic status, depression disparities, and financial strain: what lies behind the income-depression relationship?
Frederick J. Zimmermana, and Wayne Katonb
Health Econ. 14: 1197–1215 (2005)
The income – depression relationship: social selection hypothesis
Studies have consistently found the incidence and persistence of depression to be higher among persons with low incomes; greater income may be associated with reduced symptoms of depression. People with lower incomes may face stresses associated with poverty or with making ends meet that may trigger a depressive episode
Alternatively, depression also exercises an important influence on income and many of the other measures of socioeconomic status. Depression and/or its symptoms have been shown to be associated with reduced productivity, increased absenteeism, reduced aggressiveness in job-seeking, reduced ambitions in job choice, and lower educational attainment, all of which would be expected to have a downward effect on income. Accordingly, one could model some of the psychosocial determinants of economic status as

There are three distinct possible causal directions, which are not mutually exclusive:
(1) Low economic status causes depression (sometimes called the social causation hypothesis).
(2) Depression causes low economic status (sometimes called the social selection hypothesis).
(3) Some third variable(s) – possibly unobserved – cause(s) both depression and low economic status.
Early-onset depression can lead to reduced educational attainment
(Berndt ER, Koran LM, Finkelstein SN et al. Lost human capital from early-onset chronic depression. Am J Psychiatry 2000; 157: 940–947).
Depression in adults reduces work productivity
(Berndt ER, Finkelstein SN, Greenberg PE et al. Workplace performance effects from chronic depression and its treatment. J Health Econ 1998; 17: 511–535).
Treating depression improves productivity and reduces work absence
Kessler R, Greenberg P, Mickelson K, Meneades L, Wang P. The effects of chronic medical conditions on work loss and work cutback. J Occup Environ Med 2001; 43: 218–225. [4,30,31]
Zhang M, Rost KM, Fortney JC. Earnings changes for depressed individuals treated by mental health specialists. Am J Psychiatry 1999; 156: 108–114.
Simon GE, Barber C, Birnbaum HG et al. Depression and work productivity: the comparative costs of treatment versus nontreatment. J Occup Environ Med 2001; 43:2–9.
Results: The regression analysis of depression symptoms on income provides evidence only of an association, and does not imply anything about causality. Previous research has framed this issue (income – depression relationship) in terms of alternative hypotheses of social causation. (low SES is a risk factor for mental health problems) and social selection. (mental health problems lead to lower economic status). The overall direction of this research has been to suggest that both mechanisms are at work.
Earnings changes for depressed individuals treated by mental health specialists
Zhang M, Rost KM, Fortney JC. Am J Psychiatry 1999; 156:108–114.
The annual estimated income lose is $2,101 for a depressed person
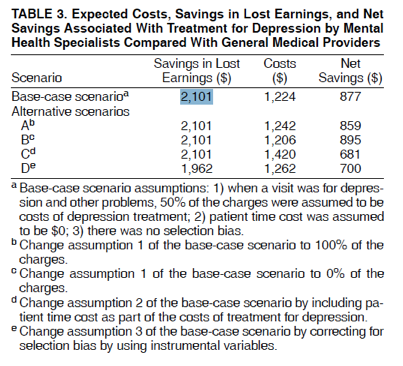
The estimated coefficient of the earnings equation indicated that the lost earnings for the average patient receiving depression treatment in the mental health sector was $2,101 lower than that of the average patient receiving depression treatment in the general medical sector during the 12-month period. In the cost equation, the expected costs of treatment for the average patient receiving depression treatment in the mental health sector were $1,224 higher than that in the general medical sector. In other words, depression treatment in the mental health sector had an average annual net savings of $877 ($2,101–$1,224) over depression treatment in the general medical sector.
Depression and Work Productivity: The Comparative Costs of Treatment Versus Nontreatment
Gregory E. Simon, MD, Catherine Barber, MPA, Howard G. Birnbaum, PhD, Richard G. Frank, PhD, Paul E. Greenberg, MA, MBA, Robert M. Rose, MD, Phillip S. Wang, MD, DrPH, Ronald C. Kessler, PhD
J Occup Environ Med. 2001;43:2 – 9
(http://www.acoem.org/health_right.aspx?id=1368)
This article discusses the impact of depression on work productivity and the potential for improved work performance associated with effective treatment.
Depression is the mental illness thought to have the largest disease burden in the general population. A growing body of evidence documents that depression is highly prevalent in the labor force and that it is associated with substantial lost productivity. Greenberg et al estimate that the annual salary-equivalent cost of major depression due to work loss and work cutback in the US labor force is $33 billion.
Using data from two nationally representative population samples of workers, Kessler et al* attempted to make a crude lower-bound estimate of the workplace cost savings associated with depression treatment by analyzing data on the relationship between severity of depressive symptoms and short-term work loss and work cutbackÉ. Depressed workers were found to have between 1.5 and 3.2 more short-term disability days per month than those without depression, resulting in a salary-equivalent productivity loss of $182 to $395 per month.
*Kessler RC, Barber C, Birnbaum HG, et al. Depression in the workplace: effects of treatment on short-term disability. Health Aff (Millwood). 1999;18:163-171.
Depression In The Workplace: Effects On Short-Term Disability Could treating workersÕ depression help employers to save money on disability? These results are encouraging.
by Ronald C. Kessler, Catherine Barber, Howard G. Birnbaum, Richard G. Frank, Paul E. Greenberg, Robert M. Rose, Gregory E. Simon, and Philip Wang
Health Aff (Millwood). 1999;18:163-171.
ABSTRACT: We analyzed data from two national surveys to estimate the short term work disability associated with thirty-day major depression. Depressed workers were found to have between 1.5 and 3.2 more short-term work-disability days in a thirty-day period than other workers had, with a salary-equivalent productivity loss averaging between $182 and $395. These workplace costs are nearly as large as the direct costs of successful depression treatment, which suggests that encouraging depressed workers to obtain treatment might be cost-effective for some employers.
Cost of Lost Productive Work Time Among US Workers With Depression
Walter F. Stewart, PhD, MPH; Judith A. Ricci, ScD, MS; Elsbeth Chee, ScD; Steven R. Hahn, MD; David Morganstein, MS
JAMA. 2003;289:3135-3144.
http://jama.ama-assn.org/cgi/content/abstract/289/23/3135?eaf
É.US workers with depression employed in the previous week cost employers an estimated $44 billion per year in LPT, an excess of $31 billion per year compared with peers without depression.



